What is Infant Colic?
Infant cramps usually appear during the first three to four months. They manifest themselves as sudden episodes of painful crying which usually occur at least three days a week, last for a week or more, and usually disappear after the age of three months. During this period, the child steadily gains weight and develops normally. In addition to crying, the child turns pale or red in the face and makes painful grimaces; the stomach is tense and bloated, the child draws the legs in, lifts the head and clenches the fists. Symptoms are more frequent in late afternoon or evening, during or after the feeding. An estimated 10 to 30% of infants suffer from cramps. The pain generally occurs in the third week, culminating in the sixth. Usually, the cramps spontaneously disappear by the end of the third or fourth month.
Why Does Colic Happen?
The precise causes of colic are not known, but they are certainly numerous. Scientific research has tested several possible hypotheses in this respect: allergy to proteins present in cow’s milk; lactose intolerance which leads to excessive gas (mostly hydrogen) which typically disappears after the third month; development (maturation) of the digestive tract (heightened intestinal activity) and the central nervous system (increased irritability); neuro-hormonal immaturity; maternal emotional tension and stressful family circumstances.
Children born prematurely with a birth weight of less than 2,500 grams are three times more likely to get cramps. Factors such as sex, socio-economic status, feeding (mother’s milk or infant formula) and family allergies do not affect the frequency of infant cramps. However, some differences do exist: cramps appear earlier if the child is formula-fed (around the second week compared to the sixth week in breastfed children) and are more frequent among children whose mothers are frightened, suffered from stress during pregnancy and birth, or smoke. Higher levels of intelligence, age and educational qualifications of the mother are also commonly associated with cramps. Moreover, first-born children experience cramps more frequently than their siblings. Considering the large number of possible causes, there is no unique treatment for cramps. However, there are some general rules that should be followed in order to reduce as far as possible the discomfort.
Health support at your fingertips
Choose: fast pediatric consultations or an AI assistant for first answers — 24/7, secure and private.
Talk to a pediatrician in real time
Video / call / chat with certified doctors. Fast, secure, and without waiting.
- Average response time < 10 minutes
- Experts across multiple pediatric specialties
- Personalized medical advice and next-step plans
Smart first steps for parents
Enter symptoms and get structured guidance on what to do — before talking to a doctor.
- Quick orientation: what’s urgent and what can wait
- Age-appropriate tips for your child
- Private: your data stays with you
Recognizing Symptoms: When to Worry
Why Colic Is So Stressful for Parents (and How to Cope)
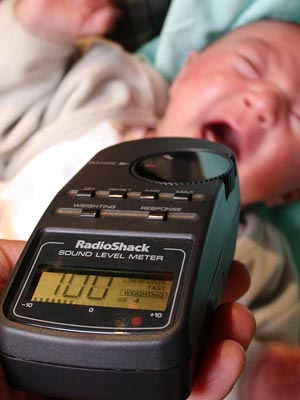
Did you know that the loudness of crying can exceed 100 dB? How loud is that? Look it up in the table below and compare!
| SOUND SOURCE | NOISE LEVEL (IN DECIBELS) | HOW WE EXPERIENCE THE SOUND |
| 0 | silence | |
| falling leaf | 0-10 | almost inaudible |
| ticking clock | 20 | borderline audible |
| light rain | 30 | very quiet |
| whisper | 40 | quiet |
| normal conversation | 50 | medium quiet |
| lecture | 60 | rather loud |
| city traffic | 70 | loud |
| loud music | 80 | very loud |
| jackhammer | 100 | very loud to unbearably loud |
| CAT 2 aircraft at a 50-metre distance | 120 | unbearably loud |
| CAT 2 aircraft in the immediate vicinity | 140 | borderline painful |
Try to think about the feelings you experience when your baby is crying. Crying is the child’s most powerful signal: it gives the parent the strongest impetus to spring into action in order to relieve the child’s discomfort. Crying can have a paralysing effect on parents who lack sufficient emotional stability. They begin to panic, behave irrationally, and are unable to create a feeling of security and comfort, thus failing the parenting test at the very first step. In fact, their behaviour creates additional unease in the child and increases the spiral of fear. Often, only one parent is frightened, so his/her partner calms him/her down, thus indirectly also calming the child.
Long-lasting cramps expose the mother to chronic stress and can lead to depression, diminishing feelings of self-worth and lack of confidence in her ability to be a good parent. The importance of the support the mother receives from her surrounding and paediatrician should therefore be emphasised. Numerous studies have shown that this type of support also has the best effect on reducing cramps. Further, it is important to create a soothing atmosphere during the child’s sleeping time (dimmed light, silence, or soft and calm music) and to respect his/her sleeping pattern. This also means avoiding situations that would create changes in the usual sleeping schedule.
In the event of frequent, strong cramps, the stool can become softer and green because of the increase in intestinal activity. Frequent pain, interrupted sleep and lack of sleep make the child irritable, which, in turn, accelerates the intestinal activity, making the cramps even more prominent. The restlessness present in the child’s surroundings (anxious parents, attempts to overcome the sound of crying in order to calm the child, shaking or frequently turning the child over) does not have a soothing effect and merely accelerates the intestinal activity (and, consequently, the cramps) even further. The child’s environment needs to be soothing: noise and bright lights should be avoided, and the mother’s voice and movements should be soft. Although it is sometimes difficult to keep calm when your child is crying inconsolably, this is the most effective way to help reduce his/her discomfort.
Parents should take turns caring for the baby: when one parent feels physically and emotionally exhausted, s/he should rest while someone else (perhaps another member of the household) takes care of the child. Avoid turning one parent into the child’s “prisoner”. This role typically befalls the mother, who should be given time to attend to her own needs, get out of the house and change her daily routine.
Movement and vibration can sometimes have a positive effect: you can try to ease the pain by rocking the child in a cradle, holding him/her as you rock in a rocking chair or on a Pilates ball, or taking him/her for a ride in the stroller (or car). Gently massaging the infant’s entire body has proven equally effective.
Breastfeeding Tips for Babies with Colic
Ensure peace for the breast-fed child and make sure s/he has hold of the entire nipple, along with the areola. With frequent and short breastfeeding sessions, the child usually sucks the “first milk” from the breast, which is rich in carbohydrates. Carbohydrates create more gas in the small intestine and are digested faster than the “second milk” which contains more fat. It is therefore recommended that the child should be fed from a single breast until s/he feels full (e.g. becomes relaxed and falls asleep) and releases the breast him/herself. Prevent “playing” with the breast by squeezing the milk out and stimulating swallowing. If the child is still hungry, offer him/her the other breast as well. Sometimes, changes in the breastfeeding position (lying, sitting, standing) can decrease the frequency of cramps.
Women with an excessive milk ejection reflex – manifested as an overly rapid flow of excessive amounts of milk which triggers coughing, choking and unease in the infant – are advised to begin breastfeeding before the infant becomes overly agitated with hunger, as sudden and energised grabbing of the nipple can trigger a strong milk ejection reflex. In cases like this, breastfeeding in a lying position may help, as gravity reduces the milk flow. If nothing else helps, try extracting a small amount of milk prior to breastfeeding or repeatedly offering the same breast (make sure you extract milk from the other breast to avoid a feeling of overflow).
Insufficient speed of the milk flow causes the child to swallow large quantities of air, which also leads to infant cramps. In cases like this, compressing the breast during feeding sessions (squeezing out the milk to increase the flow) is recommended. If nothing else helps, try offering breast milk through a bottle (a preferred alternative to using infant formula).
Bottle Feeding Tips to Reduce Colic
In the case of bottle feeding, the nipple has to have a good valve and its opening has to be large enough for the baby to draw the content without much exertion, but not so large as to enable excessive flow resulting in a mouth full of milk that is simultaneously being spilled along the nipple. At the half-way point in the meal, it is good to lift the baby on your shoulder and stretch him/her into a fully upright position (if the child remains in a reclining position, it will be more difficult for him/her to release the excess air). This will create more room in the stomach, so the feeding can continue. Repeat the action after the baby has finished the meal (with added gentle tapping on the back) to alleviate air elimination.
However, numerous tiny air bubbles still remain in the milk in the stomach, so the baby should be placed in an elevated position (45 degrees) in the baby chair or on a hard pillow for another 45 minutes in order for these bubbles to float to the top of the stomach, which will lead to air elimination. Slightly raise the mattress below the infant’s head (cca. 10 cm) to prevent excessive regurgitation. Namely, the air in the intestines increases the overall pressure within the stomach; in the case of physical exertion (caused by cramps), the pressure is further increased to such a degree that food no longer remains in the stomach but is raised towards the mouth. Acid contents of the stomach additionally stimulate the oesophagus, which may cause pain.
A paediatrician should exclude illness as a possible cause of infant colic. Allergic colitis is extremely rare among infants, so there is no need to change the mother’s or infant’s diet as soon as the cramps occur. Leave all decisions regarding possible changes in diet to the paediatrician!
Some infant formulae are intended to reduce the frequency and intensity of infant colic; however, before deciding on using them, please consult your paediatrician.
Do Medications or Probiotics Help with Colic?
Air in the intestines can be “fragmented” so as to facilitate its elimination. This is achieved by administrating simethicone (in Croatia, SAB Simplex drops) with every meal. This preparation is not resorbed, which means it is not passed from the intestines into the organism. It prevents the formation of large bubbles of gas which the intestines then try to pass (this causes pain), creating instead (much like a detergent) numerous tiny bubbles that can be passed more easily. It should be noted that research has yet to provide evidence of the indisputable usefulness of this preparation.
Probiotics are also beneficial in reducing the intensity and frequency of cramps.
The use of some “traditional” remedies such as caraway tea is not recommended as these can actually create additional gas. Other types of tea are not recommended either, especially not as remedies for breast-fed children.
If none of the recommendations listed above leads to observable improvement, consult your doctor to eliminate other possible causes of stomach pain and obtain additional treatments such as spasmolytics (antispasmodic drugs used to relieve intestinal cramps).

Skin-to-Skin Contact and Colic-Relief Positions
Skin-to-skin contact is highly effective in calming infants and reducing colic symptoms. It helps regulate your baby’s heartbeat, temperature, and stress levels while promoting bonding.
Recommended positions:
- Chest-to-chest (kangaroo care): Place your diaper-clad baby on your bare chest. Recline with your upper body elevated and cover both of you with a light blanket. This position, known as the “kangaroo method,” soothes and comforts your baby.
- Face-to-face lap position: Sit with your feet supported and knees slightly raised (around a 45° angle). Lay your baby on your thighs, facing you, ensuring close skin contact and eye contact.
- Tummy-down (colic relief): Carry your baby lying on their stomach across your forearm or lap. Gentle pressure on the tummy can help release trapped gas.
Fathers and other caregivers can also do skin-to-skin care. Studies show babies often respond equally well—or even better—to a father’s chest warmth and comfort.
Additional tip: During inconsolable crying, gently bend your baby’s knees towards their tummy to relieve pressure. Avoid invasive techniques such as inserting objects into the rectum; instead, focus on comfort and natural gas release.
Baby Massage and Gentle Exercises for Colic Relief
Gentle tummy massages and simple exercises can help soothe your baby’s digestive system and relieve discomfort.
Massage technique:
- Warm your hands and place them gently on your baby’s tummy. Take a deep breath to stay calm and relaxed.
- Massage the tummy by gliding your palms from the upper abdomen downwards. Alternate hands in a rhythmic motion.
- Draw small, clockwise circles around the belly button following the direction of digestion.
Colic relief exercises:
- Leg-to-tummy hold: Hold both legs and gently press them towards the tummy for 20–30 seconds.
- Bicycle legs: Move your baby’s legs in a cycling motion to help release gas.
- Repeat massage and exercises: Alternate between massage and leg movements in three cycles.
Perform these techniques daily for at least two weeks. While some babies respond faster than others, consistency is key to reducing colic discomfort.
Need expert advice on infant colic?
Consult pediatricians online and track your baby’s symptoms easily with the Littledot app.
Start a Consultation






