Physical trauma
When a trauma occurs, the first person to assist the child is usually someone without medical training.
Assistance from someone with basic first-aid training and a calm demeanor is often sufficient until the emergency medical team arrives. However, the mortality rate among children following physical trauma is on the rise.
The leading types of injuries in childhood include bleeding, blows to the head, and fractures.
Injuries and blows to the body, and fractures
The injuries in the heading above can be divided into the following categories:
- bleeding or skin injuries (abrasions and larger wounds, e.g. bruises, stab wounds, cuts, amputations, etc.)
- injuries and blows to the head
- muscle injuries (pulled muscles, ruptures, etc.)
- joint and tendon injuries (contusions, strains and dislocations)
- fractures
Bleeding – How to stop it quickly and effectivel
Falling down, especially on children’s playgrounds, can cause minor to heavy bleeding which demands first-aid treatment.
Minor falls usually cause small or large abrasions. They don’t bleed much but can cover a large area. Although the child is not in danger of bleeding, this type of wound can easily become infected.
To prevent infection, clean the wound properly. First, wash your hands and wear sterile gloves. Then, rinse the wound thoroughly to remove dirt. Finally, apply an antiseptic. The wound can be rinsed with a 3% solution of hydrogen peroxide or an Octenisept solution. For surface grazes, 10% Betadine (a brown iodine solution) can also be used. The surface of the wound should be covered with a sterile gauze, which is then tightened with a bandage to prevent further capillary bleeding.
Look for signs of infection such as redness or pus. Also, check if the child is vaccinated against tetanus, especially if dirt entered the wound..
Darker blood flowing continuously may indicate venous bleeding. If the blood is lighter and spurting, it could be an arterial hemorrhage. In both cases, it is necessary to first clean the wound and then apply compression to stop the bleeding. Compression can be achieved by pressing the wound itself (if it covers a smaller area) or the larger artery leading the blood to the injured area (Figure 1).
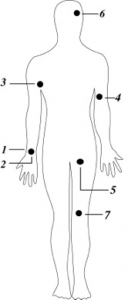
Figure 1. Compression points for stopping a heavy haemorrhage
It should be noted that attempts to stop the bleeding in this way are best left to persons with previous experience.
Once the bleeding stops, cover the wound with sterile gauze and secure it with a bandage. You can attach a small, lightweight object for additional compression. This creates additional pressure on the ruptured blood vessel, but not to such a degree that it would cut off circulation in the area below the injury.
Warning do not apply pressure on fractures
• For suspected fractures, avoid compression.
• Never press on open fractures, as sharp bone fragments can cause further internal injuries.
• Instead, immobilize the limb and seek medical help immediately.
Nosebleeds – A common but Manageable occurrence
Although seemingly harmless, this common type of bleeding frequently encountered in children’s playgrounds or sports facilities needs to be stopped. First of all, try to calm the child and those around the child, as nose bleeds typically look much more dramatic than they actually are. The child should be sitting upright and facing forward (this is contrary to the widely-held belief that the head should lean back) which will prevent the child from swallowing blood. Use two fingers to apply pressure to both nostrils for at least 10 to 15 minutes. Placing a cold compress on the back of the child’s head also helps reduce the blood flow. The child should be encouraged not to cry too much or attempt to blow his/her nose as this will only lead to more excessive bleeding and cause damage to the mucosa and blood vessels.
Head injuries – When to seek medical attention
This group of injuries is very common, especially at the earliest age, due to unexpected falls from changing mats, as well as falls which accompany the process of learning how to walk. It is important first to calm the child (and those around, too) and assess the amount and severity of the injury. If the child has lost consciousness, begins to vomit, or has a wound which requires medical attention, contact your doctor without delay.
Since internal bleeding of the head can be very slow and gradual, it is important to know that changes in consciousness or other neurological problems may occur several days after the blow to the head; when this happens, contact your doctor.
Fractures – Recognizing and managing broken bones
Our modern way of life has seen a rise in the number of children with increasingly severe fractures. The greater speed of traffic and less time parents can devote to supervising the child all contribute to this. In the case of bruising or distortions to the muscle or soft tissue, it is important also to consider the possibility of fractures.
Some signs which almost certainly point to a fracture include:
- abnormal mobility, accompanied by severe pain and deformations along the vertical axis of the limb
- audible sound of bone crepitation (bone “grinding”).
Indicative signs of fracture:
- swelling
- pain when pressure is applied
- moving the injured body part causes pain
- changes in skin colour (the result of bleeding)
- muscle spasms as an expression of the organism’s self-protection function; reduced function or its complete cessation.
Suspected fractures should be referred to a doctor – a child surgeon who will make a diagnosis with the aid of radiology. In the case of a clear external fracture it is important to stop the bleeding (if possible), cover the wound with a sterile gauze, immobilise the limb and contact emergency medical services.
If driving the child to the hospital, immobilize the affected area carefully. This prevents the bone fragments from shifting and causing more damage. This helps prevent injuries to other structures surrounding the fracture. Depending on their degree, fractures can be treated either in a conventional manner (without an operation) or with an operation.
Burns – First aid and prevention
Burns constitute a large amount of childhood injuries, frequently caused by parental inattentiveness or negligence. Unlike wounds, burns are much easier to prevent. To prevent them, it is important to pay attention to all the potential sources of burns, even as banal as a cup of coffee left within the child’s reach. If a child gets burned:
• Remove clothing and jewelry from the affected area.
• Cool the burn under running water for 10 to 30 minutes.
• Do not apply ice, creams, or butter.
• Seek medical attention if the burn is severe.
High temperatures damage tissue, releasing harmful chemicals that can spread to unburned areas. Cooling causes the blood vessels to contract, thus preventing a significant spread of these compounds into the surrounding tissue. This finally results in a smaller scope and intensity (severity) of tissue damage. Once you have cooled it, cover the burned area with a sterile gauze, give the child pain killers and contact your doctor. Despite various recommendations, avoid applying oils or ointments to the burned area as they will only obstruct the cooling process.
Download LittleDot – Your Trusted Family Health Partner!
Easily manage your family’s health with our app. Track medical records, consult doctors, and stay one step ahead. Everything you need, right at your fingertips. Download now and try it for free!